At the core of health system strengthening is the need to improve the ability of health systems to deliver high-quality services that are equitable, affordable, and accessible for all. To achieve this, health system strengthening needs to address the verticality of service delivery and weak governance structures. Poor primary health care delivery is a major challenge in many countries including Nigeria. One solution that has been proposed to address this problem is management capacity building, which aims to improve the quality and efficiency of primary health care through improved management abilities and skills. Management Capacity Strengthening is an important part of any health system development strategy as part of the effort to address some of the challenges impeding the efficiency of primary healthcare delivery in Nigeria.
Primary Health Care (PHC) is the first point of contact between people and the health system. The paucity of well-trained human resources is a major concern at the PHC level in Nigeria. One of the greatest challenges faced by front-line health workers in rural areas in Nigeria is an absence of adequate management capacity. The demographic and economic scenario of Nigeria has changed drastically since independence. Primary health care in Nigeria has evolved through a series of historical developments. Though, it is the backbone of Nigeria’s health system but has been judged to be unsatisfactory and inadequate in meeting the needs and demands of the public as reflected by the low state of health of the population due to low-quality services, poor access to basic services and high cost of treatment among others.
In Kaduna state, there was an increasing recognition that weak management capacity at the service delivery points is impeding the state’s health system from achieving its goals. Health care service delivery in Kaduna State occurs at three levels: primary, secondary, and tertiary. The primary health care level includes 1,064 primary health care facilities spread across 23 Local Government Areas, and 255 identified ward primary health care centers, serving as referral facilities for health posts and clinics in each ward.

Deputy Officer-in-Charge of Angwan Dosa PHC attending to a patient during routine Check-up
Over the years, the Kaduna State Government has demonstrated its commitment to strengthening its health system through reforms particularly targeted at repositioning its Primary Health Care system among others. Significant investments have thus been made by the State Government and its partners in implementing the Federal Government’s PHC Under One Roof (PHCUOR) policy which has contributed immensely to an improved coordination and governance environment for Primary Health Care in Kaduna State.
In plain contrast to the level of effort and investment made in strengthening the PHC system, Kaduna State has only witnessed marginal improvement in its health outcomes with consequently low impact on the health of its populace. Early efforts at diagnosing the root cause of this problem revealed that although the state has strong central coordination mechanisms for its PHC system, the lack of significant improvement in health outcomes could be largely attributed to weak governance and coordination at the PHC facility level. This is demonstrated by huge gaps in the management capacity of PHC Officers-in-Charge leading to operational inefficiencies at the service delivery points.
Evidence from a formative study conducted to inform the development of the Kaduna State PHC Management Strengthening Plan points out inherent gaps within the PHC system in the state. Some of the identified management capacity gaps for service delivery in the state include poor performance management systems, weak management capacity, frail institutional processes, weak governance structure, and a lack of enabling environment characterized by inadequate resources to effectively support quality service delivery.
As part of the efforts to strengthen the underperforming PHC delivery system in Kaduna state, Technical Advice Connect (TAConnect), in response to a Technical Assistance (TA) request from the Kaduna state government deployed systems development and capacity-building interventions to address gaps in PHC management for quality service delivery. With funding from the Bill and Melinda Gates Foundation, TAConnect engaged a consortium of the Health Strategy and Delivery Foundation (HSDF) and Solina Centre for International Development and Research (SCIDaR) to support the implementation of the Kaduna State Primary Health Care Management Capacity Strengthening Project, while working closely with the state government through the state Primary Health Care Board in March 2020.
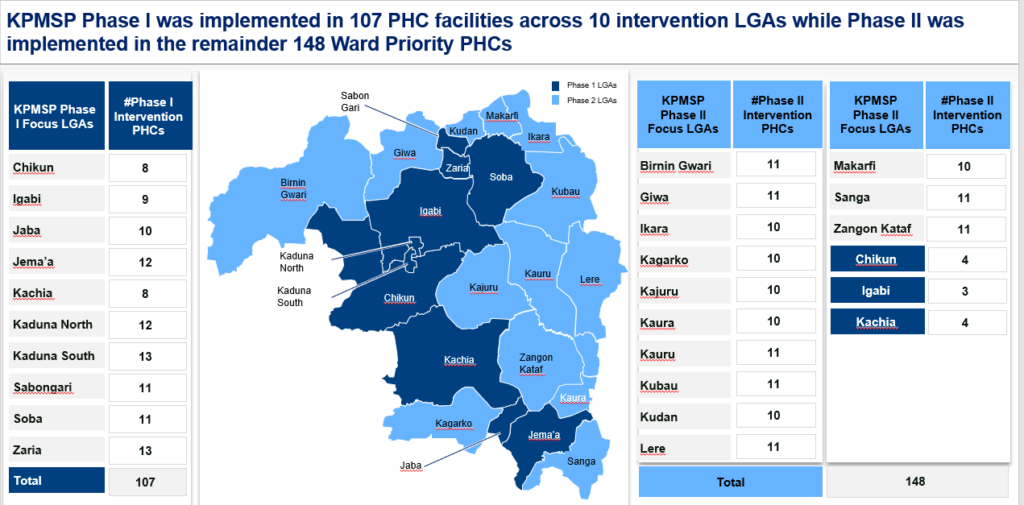
The goal of the Kaduna State PHC Management Strengthening Project (KPMSP) is to improve the management capacity of PHC Managers (also known as Officers-in-Charge (OICs)) through systems development and capacity building interventions; thereby addressing the operational inefficiencies of PHC Managers in providing quality healthcare services at the PHC facilities. Project was implemented in 2 phases, across 255 focal PHC facilities, in all 23 local government areas of the state, targeting PHC managers. Phase I of the project was implemented for 18 months, from March 2020 to August 2021, with the Phase II of the intervention which layered on systems built from Phase I, commenced from October 2021 to September 2022.
Following intensive orientation as part of the intervention, Job Descriptions and a Competency Framework were developed and officially rolled out to the PHC facilities. A stratified capacity-building plan for the management training of PHC Officers In Charges (OICs) was also developed in collaboration with the SPHCB and SICHST. Other early accomplishments of the project include the development of a consolidated handbook for OICs’ management and administrative functions and a fit-for-purpose curriculum for PHC OICs which was developed by curriculum experts and validated by the state.
In the 1st phase of the intervention, TAConnect supported HSDF to provide training for a total of 214 PHC Managers across the 10 focus LGAs within the milieu of the system strengthening component of the intervention. No fewer than 148 OICs also benefitted from in-class sessions conducted in three batches in the 2nd phase of the project concentrating on the capacity-building pillar with intensive stakeholder engagement and management.
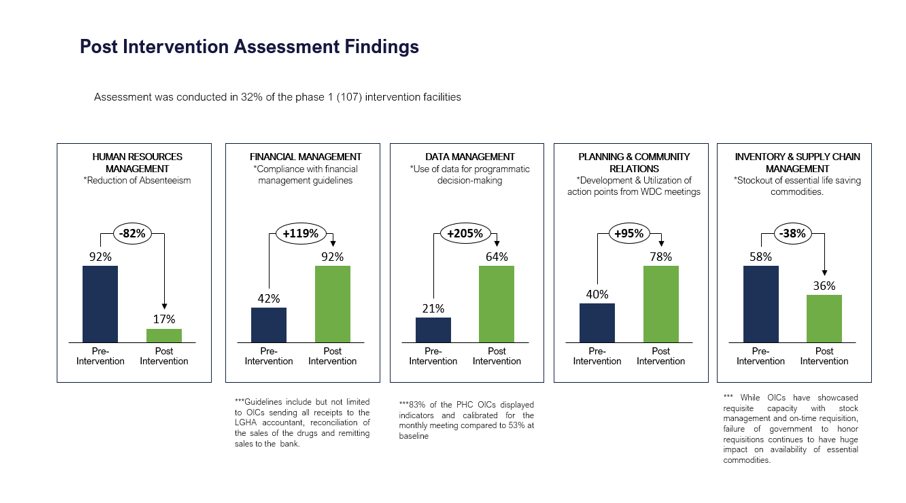
A post-intervention assessment conducted at the end of Phase I implementation to measure the impact of the intervention on the competencies of PHC OICs and PHC operational efficiencies across the five KPMSP management themes signals a degree of change on how PHCs are being managed with positive impact recorded across data management, human resource management, planning/community relations, financial management, supply chain, and inventory management.
According to the Executive Secretary, Kaduna State Primary Health Care Board, Dr. Hamza Abubakar, the intervention has triggered major innovations within the PHSC system in the state.
The new insight gained has informed the SPHCB to conduct “Management Team Leg Work” – We have made it a case in point for Management at both Headquarters and Zonal offices to visit a series of PHC facilities every quarter to do a makeover of Human Resources, Service Delivery & Infrastructure. I have learned a lot more from the KPMSP than the OICs themselves. This entire exercise has created an avenue for us to engage directly with the Facility Managers. It has shown us that the Primary Health Care Under One Roof [PHCUOR] as we previously implemented it, did not percolate down to the PHC facilities. It was essentially limited to the Zonal and LGA levels. He said.

The intervention has also helped in developing managerial competencies of PHC Managers thereby improving sound decision-making and problem-solving capabilities and enhancing patients’ experience. PHC managers have been observed to be maintaining high standards in terms of ethics and better communication. Effective coordination is palpable with symbolic self-improvement among PHC staff through the various training programs provided under both pillars of the intervention.
Since the commencement of KPMSP, my staff have become very serious with their work. They always call to seek permission if there is a very important thing that will hinder them from coming to work. This is unlike before when anyone can just decide to stay at home, sometimes for days and when they finally come, they will just be giving excuses.
-Hauwa Dawai, fficer-in-Charge of PHC Mando.
The outcome of TA Connects investment in Kaduna state has shown that addressing the need for management capacity building in the health sector is a key solution to the problem of poor primary healthcare delivery. TA connect supports national and sub-national governments to strengthen their health systems through the procurement of innovative and cost-effective Technical Assistance (TA) services.


